Your new post is loading...
 Your new post is loading...

|
Scooped by
nrip
|
The IMPACT (vIrtual-first Medical PrActice CollaboraTion) initiative, developed by the American Telemedicine Association and the Digital Medicine Society (DiMe), has unveiled a formal definition for virtual first care (V1C), along with some vignettes from providers who are only using virtual platforms to deliver emergency, respiratory, cardiac and sleep care. As set forth on the IMPACT website, virtual first care is defined as “medical care for individuals or a community accessed through digital interactions where possible, guided by a clinician, and integrated into a person’s everyday life.” The Boston-based initiative was borne out of the massive shift to telehealth during the coronavirus pandemic, and a resulting transition to hybrid care as COVID-19 eases off. In that landscape, some providers are thinking of either launching virtual-only care or transitioning their in-person services to virtual platforms. “Virtual first care is digital health in practice,” IMPACT Co-Founder Don Jones, a former Qualcomm Life executive and former chief digital officer at the Scripps Research Translational Institute, said in the press release. “IMPACT uniquely convenes organizations from across the ecosystem that view virtual first care as their primary mission. Members of IMPACT are already demonstrating patient and provider satisfaction, as well as pathways to cost savings and improved outcomes.” “With a clear definition for the field, we have paved the way for more fit-for-purpose reimbursement models and opportunities to demonstrate the value of virtual first in practice,” he added. read more at https://mhealthintelligence.com/news/mhealth-collaborative-unveils-new-definition-resources-for-virtual-first-care

|
Scooped by
nrip
|
The pandemic has accelerated some trends here, notably telemedicine. That’s given a healthy push to an emerging field – remote diagnostics. Your phone is gradually – with some extensions – turning into a remote diagnostic tool to replace doctor visits and expensive tests. That’s fairly well known, even if it is extraordinary: blood oxygen levels are captured by a device costing less than $20, while an always-on cardiac monitor tracks heart activity, for example. But that’s just the very tip of the iceberg. Remote diagnosis can transform the entire scientific basis of modern medicine. Currently, the gold standard for testing the safety and efficacy of treatments is the randomized control trial (RCT), in which some part of the trial group is treated while another part is not. Both are tracked to see whether the treatment worked, and to look for adverse events like additional illness or even deaths. Outcomes are assessed using standard statistical tools to compare the two groups. This is the gold standard. But it is based on a single core assumption: that humans by and large react similarly to treatments, and hence that the best way to address disease is to identify treatments that work effectively for large numbers of patients. Ideally, treatments work for everyone, although sometimes RCTs and subsequent tracking find groups for which a treatment doesn’t work, or another for which it works especially well – maybe the old (or young), men (or women), or people with specific pre-existing conditions. Still, this is definitely mass-oriented medicine: it’s based on the impact of treatments on what might be called the median patient. Amazon is about to enter healthcare in a big way. It is already planning to offer Amazon Care (its primary care system organized around telehealth) not just to its 1.2 million employees, but to other employers as a service, much like it offered Amazon Web Services 15 years ago (and AWS is now the leading provider of internet infrastructure in the world). It also purchased Pillpack and set up Amazon Pharmacy to deliver medications and other health products online for delivery. But the real revolution is coming inside the home. The Amazon Halo is a new health monitoring device (with some admittedly creepy privacy-related features). It is designed to apply the capabilities of AI to the needs of individual patients. And then there is Alexa, which is clearly going to be Amazon’s device of choice for wellness in the home. It’s already partnered with Sharecare to provide automated advice on 80,000 wellness and health questions, as a first line response to health concerns. Alexa will likely expand, gaining the capacity to integrate remote diagnostics and escalation into Amazon’s wider telehealth network. Still, this mostly sounds like more of the same: using telehealth and the telemedicine capabilities, but mainly just extending what we do now, making it all a bit more convenient – possibly, a lot more convenient. But all these new tools, and especially diagnostics tools, make truly personal medicine possible – like Amazon, all this will be individual-specific: a market segment of you. read the entire unedited article at https://www.healthitanswers.net/into-the-future-amazon-and-the-coming-rise-of-personal-healthcare/

|
Scooped by
nrip
|
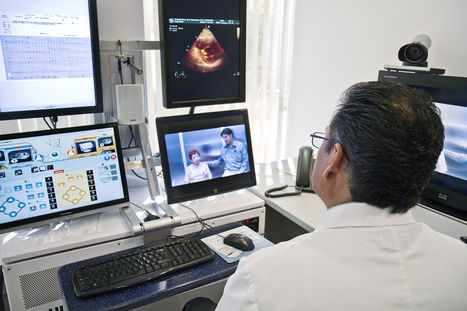
Previous work has specifically described the potential for using telemedicine in disasters and public health emergencies. No telemedicine program can be created overnight, but U.S. health systems that have already implemented telemedical innovations can leverage them for the response to Covid-19. A central strategy for health care surge control is “forward triage” — the sorting of patients before they arrive in the emergency department (ED). Direct-to-consumer (or on-demand) telemedicine, a 21st-century approach to forward triage that allows patients to be efficiently screened, is both patient-centered and conducive to self-quarantine, and it protects patients, clinicians, and the community from exposure. It can allow physicians and patients to communicate 24/7, using smartphones or webcam-enabled computers. Respiratory symptoms — which may be early signs of Covid-19 — are among the conditions most commonly evaluated with this approach. Health care providers can easily obtain detailed travel and exposure histories. Automated screening algorithms can be built into the intake process, and local epidemiologic information can be used to standardize screening and practice patterns across providers. Much medical decision making is cognitive, and telemedicine can provide rapid access to subspecialists who aren’t immediately available in person. Recognizing that patients prioritize convenient and inexpensive care, Duffy and Lee recently asked whether in-person visits should become the second, third, or even last option for meeting patient needs read the original article at https://www.nejm.org/doi/10.1056/NEJMp2003539

|
Scooped by
nrip
|
The University of Cincinnati has invented a new telehealth drone to improve access to medical services regardless of location. Researchers at the University of Cincinnati are creating a drone that can make telehealth house calls. Three colleges at the University of Cincinnati collaborated to develop a semi-autonomous drone that can be dispatched right to people’s homes. The drones are big enough to carry medicine or medical supplies but small enough to maneuver the tight confines of a home using navigational algorithms developed by UC engineers so patients can talk face to face to their doctors or pharmacists. Still in development, the drone has cameras and a display screen so patients can talk to health care professionals from the comfort of their home. The prototype carries a waterproof box the size of a small first-aid kit to deliver medical supplies or collect self-administered lab tests. “Most drones rely on controllers that work on radio communication and require line-of-sight for safe, remote operation. That’s why most drones have limited operational range,” said Manish Kumar, a professor of mechanical engineering. “If you want beyond line-of-sight control, you need some autonomous capabilities,” His lab has been working on autonomous systems that combine artificial intelligence with a suite of sensors that allow drones to navigate a cluttered and complex three-dimensional environment, like the entrance to a person’s home and living room. Further, Debi Sampsel, director of telehealth at UC's College of Nursing, quoted "When COVID-19 hit, telehealth emerged as a prime way to talk with healthcare professionals and receive certain types of therapies. Telehealth is here to stay" “We can perform all kinds of functions: chronic disease management, post-operative care monitoring, health coaching and consultations,” she added. “And in the health care arena, there is no age limit. Telehealth services are useful from birth to death.” Sampsel has been working on connected health concepts for several years at the university, and helped to develop a “smart house” to test the technology for seniors and those with disabilities. Read more at the University of Cincinati's website https://www.uc.edu/news/articles/2021/03/virtual-medicine--new-uc-telehealth-drone-makes-house-calls.html#main

|
Scooped by
nrip
|
We are directionally headed towards a significant shift in the way care is delivered. The rapid up scaling of virtual care capacity and the mainstreaming of Telehealth have given rise to new digital health tools. Self-triaging and contact tracing for COVID-19 infection detection are among the new breed of digital health applications that startups to big firms alike were looking at to seize the emerging opportunities. Telehealth is here to stay. Healthcare is shifting to virtual care models. Digital front door apps are all the rage. What else is emerging that could change the way we experience care? While telehealth is now the de facto mode of accessing healthcare for most low-acuity and routine care needs, a number of related technology-led trends are quietly gaining ground as well. Here the author looks at a few of these and opinionates on their potential impact on healthcare consumer experiences. "contactless" experiences: Covid has made us all afraid to touch any surface exposed to the public. Nowhere is this fear more prominent than a hospital or clinic setting. Healthcare executives now speak of airport check-in type of experiences for healthcare appointments, both for in-person and virtual visits. Technology-enabled workflows now enable patients to complete most of the registration formalities prior to the visit, be it a virtual consult or a clinic visit. Registration kiosks in hospital lobbies may soon be enabled with facial recognition software to eliminate the need for touching any surface. Routine examinations are also going virtual, with many diagnostic procedures now possible through remotely controlled devices. Caregivers are beginning to do their patient rounds through virtual visits. This trend will only grow in the coming years. Contact tracing Inspired by the success of India, Singapore and South Korea, contact tracing applications on Bluetooth-enabled devices have been positioned as an effective means to track and trace infections to reduce the spread of COVID-19 Despite many setbacks, contact tracing's potential for deployment within communities and populations for uses beyond COVID-19 has longer-term potential, and this could be the single most important technology-enabled healthcare program to come out of the COVID-19 crisis. Remote monitoring and automated communication Healthcare executives are more motivated than ever to keep their populations healthy in their homes. A vast and growing array of automated communication tools allows caregivers to use rule-based messaging to push everything from health coaching, post-discharge care instructions, and appointment reminders through IVR, text, SMS, and mobile alerts. Data mining tools can identify subsets of populations at risk and enable caregivers to intervene on time. A New York-based COVID-19 Rapid Response Coalition involving tech giant Amazon that targeted high-risk populations through SMS campaigns that reached up to 10,000 members a day, is an example of how automated communication tools can serve populations in a crisis and during normal times. The use of digital health and automated communication tools has also improved healthcare outcomes by reducing no-shows for appointments, increased adherence to medication regimens, and targeted interventions during adverse events. There is an unprecedented opportunity today to use telehealth technologies in the complete continuum of care. However, healthcare enterprises and their technology partners need to make them more user-friendly. That will determine success for new technology-enabled virtual care models. Every health system has to design the digital experience that is suited for their patient populations while remembering to address the needs of caregivers who will deliver and manage the experiences.

|
Scooped by
nrip
|
The concept of telemedicine is still in its infancy, but has some appeal to doctors and patients, especially in rural U.S. communities where doctors have great distances to cover for short in-person patient visits.
Medical technology watchers know the ‘telemedicine’ concept isn’t as far-fetched as it would have sounded a decade ago: patients can now connect with a doctor from home or a clinic using a web cam, and the provider can offer a basic diagnosis, a referral or a prescription. The concept is still in its infancy, but has some appeal to doctors and patients, especially in rural U.S. communities where doctors have great distances to cover for short in-person patient visits.
A Cisco study from last spring showed that a majority of 1,547 customers from 10 countries are willing to embrace this direction in health care. As many as 74 percent said they would be comfortable talking with their doctor in other ways besides in person, such as email, text, or video chat, and 80 percent of surveyed residents from North America said they’d feel comfortable with their medical information shared online.
In-person visits aren’t going away immediately, but more and more advantages are in the spotlight for using cutting edge technology:
Read more: http://www.33rdsquare.com/2014/01/4-reasons-why-telemedicine-may-be-here.html

|
Scooped by
nrip
|
The doctor isn’t in, but he can still see you now.
Remote presence robots are allowing physicians to “beam” themselves into hospitals to diagnose patients and offer medical advice during emergencies.
A growing number of hospitals in California and other states are using telepresence robots to expand access to medical specialists, especially in rural areas where there’s a shortage of doctors.
These mobile video-conferencing machines move on wheels and typically stand about 5 feet, with a large screen that projects a doctor’s face. They feature cameras, microphones and speakers that allow physicians and patients to see and talk to each other.
“Regardless of where the patient is located, we can be at their bedside in several minutes,” said Dr. Alan Shatzel, medical director of the Mercy Telehealth Network. “Literally, we compress time and space with this technology. No longer does distance affect a person’s ability to access the best care possible.”
|

|
Scooped by
nrip
|
The pandemic drove many patients to their primary care docs via video. And it worked. A telehealth expert (Dr. Peter Antall) explains how this shift could become a permanent hybrid with in-person care in an Interview with healthcareITNews Here is a summary from the interview. What is Virtual Primary Care Virtual primary care is allowing patients to see their primary care physician in person or virtually, depending on their needs. It combines the convenience of telehealth with the ability to strengthen recurring relationships with primary care physicians. It also can help provide a medical home for patients who have no primary care physician, either due to lack of access or lack of engagement. The emergence of virtual primary care stems from the recognition that the traditional primary care model doesn't work well for many patients. Access to care remains a major issue for many patients, due to geographical constraints and a growing shortage of primary care physicians, which has only been exacerbated by the pandemic. Do Patients Want it? Patients are receptive. A recent Amwell survey shows consumers want a virtual approach to primary care – - Most consumers (77%) would prefer to see their existing primary care provider via video.
- 25% of consumers are willing to switch providers to get it.
- 80% saying they would prefer to see the same primary care physician regularly via virtual care.
Can virtual primary care provide a simple, seamless care experience? How are patients supported throughout the care process? The best virtual primary care programs are well coordinated and enable a seamless care experience with the ability to transition patients between in-person and virtual care settings, and to various specialties or allied care providers as needed. In this way the care is holistic and the patient journey is clear and simple. Data sharing is an important part of creating a highly coordinated and seamless care experience. Records from all visits should be available to all providers on the telehealth platform across specialties and should be shared with the primary care physician in brick and mortar if one exists. This interoperability improves care and improves the referral and transition process. To ensure patients are supported, virtual primary care programs should include care coordination capabilities. For example, secure messaging between patients, healthcare professionals and administrative staff can help patients receive quick answers to their questions and ensure that all of their needs are met in a timely fashion, even after a visit has finished. Can virtual primary care help with population health? The flexibility of remote access makes it possible for providers to see patients' living conditions, evaluate social determinants of health, and respond in ways that make a deep impact on patients' lives. Providers also can leverage virtual primary care to evaluate medication adherence among patients with diabetes, hypertension and high cholesterol. When breakdowns in medication adherence are discovered, providers and support staff can work to engage patients in following their treatment plan more closely. This avoids complications that can occur when patients deviate from recommended treatment. Improvements in compliance and ongoing care can be accomplished through use of frequent brief touchpoints, care coordination, nudges and team-based care. Prompts and reminders can be used to reinforce the care plan. With capabilities such as these, virtual primary care positions providers and health plans not only to improve population health, but also to perform well under value-based models of care. More and more, it's clear that the future of care depends on hybrid models of care delivery such as this and I believe we've only just begun to scratch the surface of what's possible with virtual primary care and how it contributes to the continued transformation of healthcare. read the unedited article on the interview at https://www.healthcareitnews.com/news/will-virtual-primary-care-become-new-model-healthcare-delivery

|
Scooped by
nrip
|
The aim of the Connected Healthcare Study was to understand the impact COVID-19 has had on health care and communication with providers and gain insights into experiences and preferences as it relates to telehealth and online health care tools. More than two-thirds of U.S. patients (69%) had seen a health care provider via telehealth since the COVID-19 pandemic began, with more than two in five (46%) meeting with a PCP and about one in five (19%) meeting with a mental health care provider. Other providers whom respondents have seen via telehealth since the pandemic began included specialties like ophthalmology and women’s health and orthopedic care, which were not considered typical telehealth users before the pandemic. Telehealth is clearly emerging from the COVID-19 pandemic as the new normal – an overwhelming majority (84%) of respondents who received telehealth services since March 2020 reported that they plan to continue using telehealth appointments in the future, with the top reasons being that it’s more convenient (43%) or to avoid being around people who are ill (39%). One of the most striking results of the survey was that nearly half of U.S. patients (48%) reported that they have sought (4%) or would be likely to seek care (44%) from a different health care provider if their current provider did not offer telehealth appointments. This is clearly a resounding message of support for telehealth from patients to their physicians. As we look back on the broader impact of the COVID-19 pandemic, it will have catapulted patient awareness and acceptance of telehealth and virtual care to the extent that would have been inconceivable before the pandemic. It has also brought to the forefront many other aspects of patient electronic and virtual engagement with providers across all specialties. read the entire post at https://www.kevinmd.com/blog/2021/05/how-do-patients-really-feel-about-virtual-care-and-electronic-patient-engagement.html

|
Scooped by
nrip
|
If there’s one dialogue that’s been growing louder across the healthcare landscape, it’s the consumerization of healthcare. Market trends are undeniably steering the healthcare experience into a new paradigm where patients are seizing control. Yet this new direction is not always beneficial for patients or providers. Just as consumer-driven industries like Uber and Netflix offer quick and seamless digital transactions, many patients want greater convenience and speed from care delivery. Many are also seeking more cost-effective options, thanks to climbing medical debt and high-deductible insurance plans. They’re less willing to tolerate care delays and inefficiencies; many will leave a poor online review after a frustrating appointment. These are all understandable goals and reactions. But as patients climb into the driver’s seat of healthcare, they’re not always given a roadmap to their intended destination. As they navigate their options, some are running up against four dynamics: 1. Dr. Google In our fast-paced world, many patients don’t want to wait weeks for an appointment or take time off from work to bring their child to the pediatrician. Instead they take out their smartphone and look up symptoms to get a quick and theoretical diagnosis. Patients can view photographs of lesions, read checklists of cancer symptoms and lurk on forums where people describe surgery experiences – and encourage each other to self-diagnose.
2. Retail Clinics
Retail clinics like CVS and Walgreens have exploded in popularity – and the market is expected to surpass $8 billion USD by 2028. Patients who feel they’re too busy or too peripatetic to maintain a consistent PCP relationship often prefer the extended hours and easy access of these clinics.
3. Cost Avoidance
Patients are paying higher and higher coinsurances, deductibles and copays – and they’re sick of it. They’re annoyed by a hospital’s inability to give them an accurate procedure cost in advance; many are stuck with “surprise” invoices after checking into a network hospital and receiving care from an out-of-network doctor.
4. Application Chaos
As applications and portals take over the Internet, many healthcare systems have turned a great idea into patient confusion. Even patients with moderate care needs may find themselves managing an overwhelming collection of healthcare apps for their OB/GYN practice, dentist, dermatologist, PCP, various hospital online payment portals, lab result repositories and data from their wearables.

|
Scooped by
nrip
|
Thousands of therapists are providing Tele-services to their patients during the covid imposed lockdown using video-enabled platforms like Zoom, Skype, Google Meet, etc. Many of them hadn’t intended to ever take the online route, however, a number of them are now discovering the ease of use and the convenience of it, both for themselves and for their patients. While the technological tools available for mental health professionals and patients has dramatically improved over the past decade, those transitioning to online services rapidly need to hold a few things in mind. It’s not the same as in-person therapy While online psychotherapy has been shown to be just as effective as in-person care, the delivery of psychotherapy via telehealth requires skills that in-person therapy does not. Because the skill set for online consults is different, therapists typically need additional training in telehealth. The amount of training can/will vary depending on the skills of each person. As the technology continues to get more user-friendly, the amount of training needed becomes less. The legal considerations have changed, but not in the ways some therapists think The Department of Health and Human Services is using its enforcement discretion to allow providers to use video-calling platforms, such as Zoom and Facebook Messenger, that are not compliant with HIPAA privacy rules. The Centers for Medicare and Medicaid Services have also loosened geographic restrictions on telehealth provision. But both of these moves have been widely misunderstood, and they are only temporary in nature. Ethical standards haven’t changed Certainly, many therapists had to switch to telehealth quickly and may have done so even without initial training in order to ensure continuity of care to at-risk clients. In the event of a complaint, ethics committees would likely take such factors into consideration. But therapists who have not been trained in telehealth and whose clients have not provided informed consent specific to telehealth should do so as quickly as possible. Therapist fears about negative impacts haven’t been supported by research While telehealth needs to be entered into thoughtfully, many of the reasons therapists have traditionally given for their resistance to telehealth simply haven’t shown up. For example, therapists often point to the eye contact issue described above and express concern that building a therapeutic relationship is harder online. Research hasn’t supported this idea. While therapists are sometimes less satisfied with the therapeutic relationship in telehealth, clients show no difference – and in some studies actually feel a stronger alliance in online care. Mistakes are common and avoidable Some steps one can take to avoid common mistakes include: – Choose a secure telehealth platform that offers a Business Associate Agreement stipulating who has access to confidential information and how it can be used – Learn the platform well, and practice using it with a friend or colleague to test all of its features – Understand the legal requirements surrounding telehealth in your state, and complete any state-mandated training – Always get client consent before sending private client information via an unsecured email – Review your telehealth technology and data security practices at least annually. read the original article at https://hitconsultant.net/2020/06/12/what-therapists-need-to-know-about-telehealth-technology/#.XuYlqmozZPt

|
Scooped by
nrip
|
With fear of COVID-19 keeping many routine visitors away, rural hospitals have too few patients to stay afloat financially, and virtual medicine isn't saving them. Virtual health care, in theory, sounds perfectly suited to the needs of rural populations. It kicks down the barrier of traveling great distances for medical needs and works increasingly well for diagnosing and managing the chronic and non-emergency health issues endemic to these parts of the country, such as diabetes, hypertension, asthma, and melanoma Yet success at implementing these virtual systems has been a patchwork. Unreliable access to at-home technology, broadband internet service, and cell reception have plagued some places, while ever present financial hurdles abound. Rather than usher in a long-anticipated telemedicine revolution in remote areas, COVID-19 has exposed its limitations, and highlighted what tools and regulations rural hospitals will need to survive the pandemic. read this insightful piece at https://www.nationalgeographic.com/science/2020/06/why-rural-hospitals-may-not-survive-coronavirus-telemedicine/

|
Scooped by
nrip
|
72% of consumers across the eight countries are willing to see a doctor via telehealth video conferencing for non-urgent appointments, according to Intel survey.
The study, “Intel Healthcare Innovation Barometer” was conducted across eight countries by Penn Schoen Berland in Brazil, China, France, India, Indonesia, Italy, Japan and the United States from July 28 to Aug. 15, 2013 among a representative sample of 12,000 adults ages 18 and older. The findings concludes that most people are optimistic about technology innovations advancing healthcare, are open to sharing healthcare information for the greater good and receptive to using sensors for personalized care.
As the technology of remote patient monitoring solutions and mobile health applications improve, consumers now have the ability to connect with their providers in a variety of ways to embrace new behaviors
Other key findings of the Intel Healthcare Innovation Barometer include:
Improving Personal Care and Self-Monitoring with Technology - Sixty-six percent of people say they would prefer a personalized healthcare regimen designed specifically for them based on their genetic profile or biology.
- Fifty-three percent of people say they would trust a test they personally administered as much or more than if performed by a doctor.
Sharing Anonymous Digital Health Records for the Common Good - People are more willing to anonymously share their health records or genetic information than their banking information or phone records.
- More than three-quarters (76 percent) of respondents over the age of 55 would be willing to anonymously share results of lab tests or health monitoring to contribute to research databases compared with 64 percent of millennials.
- India is the country most willing to share healthcare information to aid innovation.
Emerging Technology Tools for Increased In-Home Health Management - Half of those surveyed would trust a diagnosis delivered via video conference from their doctor.
- Seventy-two percent are receptive to communication technologies that allow them to remotely connect to their doctor.
- The innovation least likely to be incorporated by the global population is a robot performing surgery.
- Almost half of respondents (43 percent) globally would trust themselves to monitor their own blood pressure and other basic vitals.
|



 Your new post is loading...
Your new post is loading...